Imagine you arrive at your morning urology list with 7 cystoscopy cases. Your 1st patient is a 60yo male for a rigid cystoscopy. He has a drug eluting stent from an AMI 5 years ago and has functionally declined since. He is 120kg with the usual collection of diabetes, hypertension and hypercholesterolaemia with no previous surgical history. He suffers dyspnoea with minimal exertion. The surgeon says that this is a straightforward stent insertion for a ureteric stone lasting approximately 15mins.

What kind of anaesthetic do you choose for this case? Do you postpone for cardiac testing, or do you proceed as it is urgent? Do you insert an arterial line or opt for standard monitoring? Do you insert an LMA or an endotracheal tube?

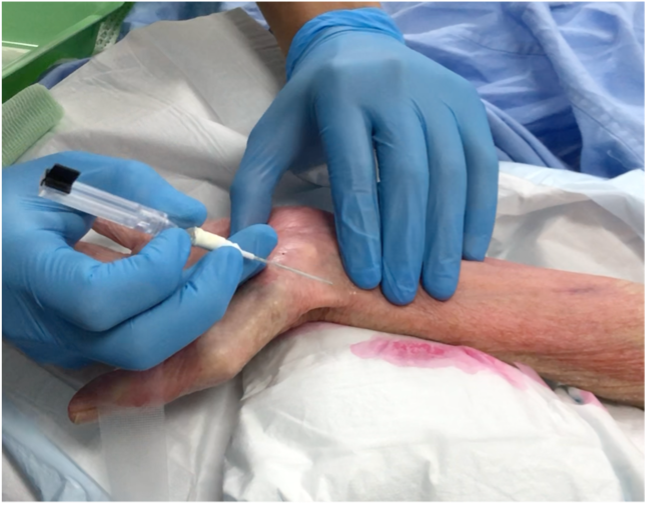
My subconscious feeling is that the anaesthesia may be more challenging and take more time than the surgery. I want you to think about this for a moment. Most of the time, the surgery takes more time, more staff, equipment and cost than the anaesthetic. When this is flipped, anaesthetists feel uneasy that they need the extra resources.
I believe that when the effort/time for anaesthesia increases beyond what is expected, this may cause an anaesthetist to feel stress and lead to standard care being provided when advanced monitoring/airway/procedures may be indicated.
Think of a typical case, such as a laparoscopic cholecystectomy. The anaesthesia preparation and induction are generally straightforward – insert an iv cannula and proceed with a relaxant general anaesthetic. Take a complex case such as a liver resection. The anaesthesia preparation and induction are expected to take more time. 2 large bore iv cannulas, an arterial line, a central line and even intrathecal morphine. Typical cases with typical anaesthesia preparation times don’t cause undue stress.
But in the cystoscopy case above, this is a short case that normally takes minimal anaesthesia preparation – iv cannula and LMA for the airway. However, you are faced with the fact that this patient may need an ETT (BMI and head down lithotomy position) and an arterial line (Ischaemic heart disease and poor cardiorespiratory function) requiring more time than normal on a busy list. Additionally inserting an arterial line/ETT is not an absolute requirement. Depending on your level of experience and skillset and patient subtleties you may not need to do these extra tasks.
If the same patient presented for a laparotomy, I would not hesitate to insert an arterial line and ETT, but the fact that the surgery is short and there are several cases on the list means I must make a subtle difficult decision about taking more time for this case at the risk of cancelling a case on the list or running over time.
This is a common dilemma worth highlighting where a complex anaesthesia patient presents for a routine/short surgical case. This often happens for plastics, urology, gynaecology cases, gastroscopies, colonoscopies and cataract operations.
I believe the crucial point is that anaesthesia and surgical risk are often mutually exclusive. If the patient requires advanced steps, interventions or procedures, and you feel uneasy due to the lower risk of the operation, do not compromise your anaesthetic!
My practical approach is to
1. Set expectations early. Inform the team/surgeon that the patient is complex and will require extra interventions and time.
2. Ask them to leave the room if you perform better without people hovering around.
3. Call for the patient early and do as much preparation during the previous case.
In this case, you thankfully choose an ETT and arterial line. After a gentle induction with lower doses of propofol, higher doses of fentanyl and muscle relaxant, the blood pressure still falls to 50mmHg. Fortunately, you can treat it immediately with a vasopressor and run an infusion. The arterial line insertion was worth the extra time allowing immediate detection of severe hypotension.
If you have found this an issue in your practice or if you have any questions, please write in the comments below!
Dr Lahiru