Dementia risk following general or regional anaesthesia
by Dr. Matthew Vella
@mjv.igee
#Anaesthesia #anaesthetics #anesthesiology #anaesthesia #anaesthetic #abcsofanaesthesia #medicine #anesthesiologist #anaesthetist #anesthetist #anaesthesiology #nurse #medical #meded #FOAMed #medicalstudent #dementia #delirium #cognitivedysfunction #generalanaesthesia #GA #regionalanaesthesia #RA #inhalational #spinal #epidural #TIVA #hipfracturesurgery #longtermanaestheticrisk #anaestheticconsent
Title:
Dementia risk amongst older adults with hip fracture receiving general anaesthesia or regional anaesthesia: a propensity-score-matched population-based cohort study
Sun, M., Chen, W. M., Wu, S. Y., & Zhang, J. (2023). Dementia risk amongst older adults with hip fracture receiving general anaesthesia or regional anaesthesia: a propensity-score-matched population-based cohort study. British journal of anaesthesia, 130(3), 305–313. https://doi.org/10.1016/j.bja.2022.11.014

Where is it published?
British Journal of Anaesthesia
Who is involved?
A research group in Taiwan with funding from the Lo-Hsu Medical Foundation
What did they set out to do?
Compare long-term risk of dementia following inhalational GA vs TIVA vs regional anaesthesia (RA), and to clarify associations (if any) between dementia and age, gender, comorbidities, ASA physical status.
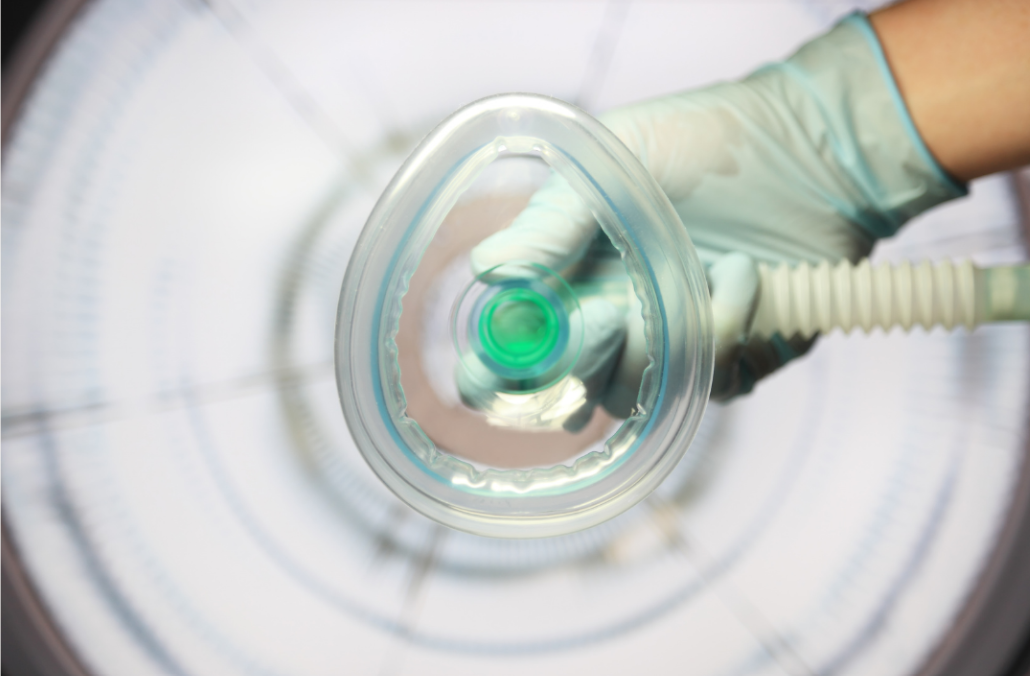
What is significant about the study?
We have an ageing population with increasing accessibility of surgery, so it’s important to understand the effect anaesthesia may have on development of dementia – considering its high morbidity, mortality, and associated healthcare costs.
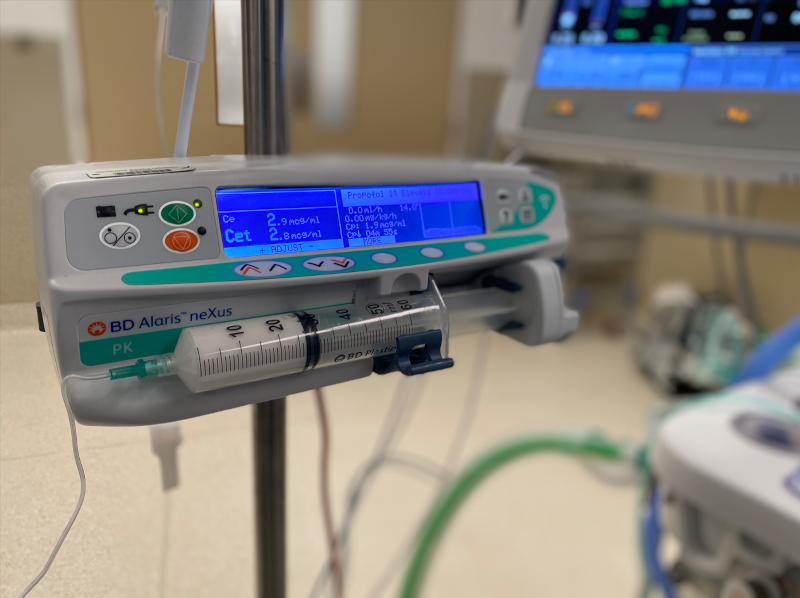
How was it done?
This was a retrospective population-based cohort study with propensity-score-matching using a huge national health database in Taiwan (National Health Insurance Research Database NHIRD) that is well validated with high data accuracy. 268, 014 patients were divided into 3 groups (inhalational GA or TIVA or Regional) and compared with regard to incidence of diagnosis of dementia.
This included patients aged over 65-years, who had elective hip fracture surgery, and were hospitalised for >1 day over 17 years (2002-2019).
Those who received a combination of inhalational and IV anaesthesia, had a history of dementia, received anaesthesia between surgery and follow-up, or passed-away, were excluded.
What did they find?
Undergoing general anaesthetic may expose people over 65-years of age to a higher risk of developing dementia in the long-term, and this risk may be mitigated by offering regional anaesthetic techniques (where appropriate).
The Details
Confounding variables were adjusted for with participants matched in a 1:1 ratio, a time-varying Cox proportional hazards model was used to quantify incidence. Statistical significance (p < 0.017 -> Bonferroni-adjusted 0.05/3). Endpoints were reported as incidence rates per 100,000 person-years and incidence ratios. Subgroup analyses were completed via multivariate time-varying Cox regression model.
Dementia incidence was significantly different between all 3 groups:
- Inhalational > TIVA > Regional anaesthesia (RA)
- Dementia risk increased over time for all groups
- For ASA 4 patients, risk of dementia was equal in all groups
Dementia incidence rates for the groups were:
Inhalational general anaesthesia (GA) 4821/100 000 person-years
Total intravenous anaesthesia (TIVA-GA) 3400/100 000 person-years
Regional anaesthesia (RA) 2692/100 000 person-years
The dementia incidence rate ratio (95% confidence intervals [CI]) were:
Inhalational GA to RA 1.19 (1.14;1.25) p = 0.011
Inhalational GA to RA 1.51 (1.15;1.66) p = <0.001
TIVA-GA to RA 1.28 (1.09;1.51) p = <0.001
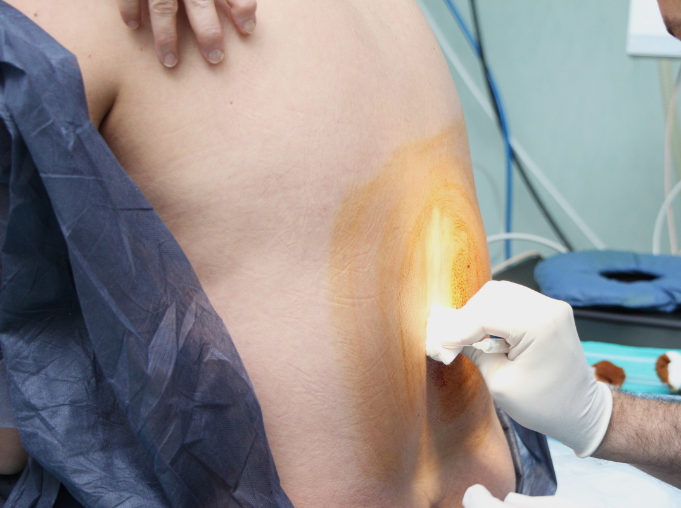
Some interesting discussion points
The current study’s findings are congruent with animal studies, where propofol shows superior post-administration cognitive outcomes compared with inhalational anaesthetic (both are implicated with increased production of AB peptides, AB amyloidosis, tau hyperphosphorylation, and neurofibrillary tangles).
Methodology was directed at improving on limitations and design flaws from prior cohort studies (i.e., insufficient sample size / follow-up, inappropriate control groups, failed distinction between dementia comorbidities, surgery type, anaesthesia type). For example, Velkers et al. (2021) (a retrospective cohort study also using propensity score matching) found no association between dementia risk and GA or RA, however they were limited by: inclusion of different surgeries, smaller sample size (i.e., 7499 per group) and short follow-up (<5 years).
Any limitations?
Only patients from Taiwanese / Asian background were included, there is potential for errors in diagnosis (ICD coding in the database), specific anaesthetic agents were not specified, and there was no specified formal testing for pre-operative cognitive impairment; so undiagnosed pre-operative cognitive impairment may have added bias.
Perhaps most significantly, as this was a retrospective cohort study, so the researchers could not determine the reason for selection of type of anaesthesia.
However, with the “propensity-score matching, no significant differences between groups were observed in age, sex, comorbidities, smoking, alcohol-related diseases, or ASA physical status. The crude dementia incidence in the inhalational GA group differed significantly from that in the TIVA and RA groups.”
What’s the overall take-home?
People may be at increased risk of developing dementia depending on the type of anaesthesia they receive, and this warrants further investigation (prospective randomised control trials). Further, it may be appropriate to include explanation of this risk as a routine part of consent.

Further reading
The RAGA Randomized Trial (delirium):
Li, T., Li, J., Yuan, L., Wu, J., Jiang, C., Daniels, J., Mehta, R. L., Wang, M., Yeung, J., Jackson, T., Melody, T., Jin, S., Yao, Y., Wu, J., Chen, J., Smith, F. G., Lian, Q., & RAGA Study Investigators (2022). Effect of Regional vs General Anesthesia on Incidence of Postoperative Delirium in Older Patients Undergoing Hip Fracture Surgery: The RAGA Randomized Trial. JAMA, 327(1), 50–58. https://doi.org/10.1001/jama.2021.22647
Retrospective cohort study with contrary findings:
Velkers, C., Berger, M., Gill, S. S., Eckenhoff, R., Stuart, H., Whitehead, M., Austin, P. C., Rochon, P. A., & Seitz, D. (2021). Association Between Exposure to General Versus Regional Anesthesia and Risk of Dementia in Older Adults. Journal of the American Geriatrics Society, 69(1), 58–67. https://doi.org/10.1111/jgs.16834
Directions for future research methodology:
Vacas S. (2023). Advancing our understanding of postoperative cognitive trajectories in older adults. British journal of anaesthesia, 130(3), 250–252. https://doi.org/10.1016/j.bja.2022.12.021